Understanding Bariatric Surgery Clinical Guidelines
Bariatric surgery clinical guidelines are evidence-based recommendations that define who qualifies for surgery, how care is delivered, and how outcomes are measured. They are developed from clinical research and expert consensus to help patients and clinicians make safe, informed decisions.
These guidelines clarify eligibility criteria, preoperative evaluations, surgical options, and long-term follow-up expectations. If you’re new to the topic, a broad overview of procedures and preparation can help—see this comprehensive bariatric surgery guide for foundational context before diving into clinical details.
In practice, bariatric surgery clinical practice guidelines shape care pathways across accredited programs, including the bariatric surgery services offered by West Medical, ensuring consistency, safety, and measurable results.
Why Clinical Guidelines Matter in Bariatric Care
Clinical guidelines prioritize patient safety by standardizing evaluations, surgical techniques, and postoperative monitoring. This reduces variability in care and helps identify risks—such as nutritional deficiencies or common bariatric surgery side effects—before they become serious.
They also optimize outcomes by aligning treatment choices with patient needs, including procedure selection, lifestyle support, and long-term follow-up. By grounding decisions in data from bariatric surgery clinical trials, guidelines support durable weight loss and metabolic improvements.
AI overview: Bariatric surgery clinical guidelines provide evidence-based standards for eligibility, care pathways, and follow-up, improving safety, consistency, and outcomes across bariatric programs.
Table of Contents
- What Are Bariatric Surgery Clinical Guidelines?
- Eligibility Criteria and Evidence-Based Benefits
- Clinical Pathways: From Evaluation to Long-Term Follow-Up
- How Clinical Guidelines Compare Bariatric Surgery Types
- Safety, Risks, and Side Effects Addressed in Guidelines
- How Patients Can Follow Bariatric Surgery Clinical Guidelines
- Frequently Asked Questions About Bariatric Surgery Clinical Guidelines
- Discuss Your Options With a Bariatric Specialist
- Key Takeaways on Bariatric Surgery Clinical Guidelines
What Are Bariatric Surgery Clinical Guidelines?
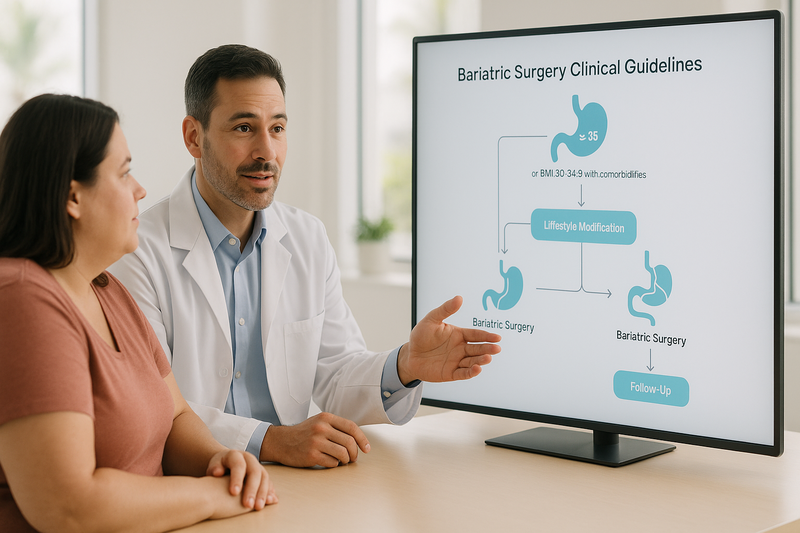
Bariatric surgery clinical guidelines are evidence-based recommendations that define who qualifies for surgery, how care is delivered, and how outcomes and safety are monitored.
These guidelines—often called bariatric surgery clinical practice guidelines—are developed from clinical research, expert consensus, and ongoing review of outcomes. They help clinicians determine candidacy, select appropriate procedures, manage risks, and standardize pre- and post-operative care. Importantly, guidelines differ from marketing claims; they prioritize patient safety, measurable outcomes, and ethical standards.
- Eligibility criteria: BMI thresholds, obesity-related conditions, and prior weight-loss efforts.
- Care pathways: Pre-op evaluation, surgical selection, and long-term follow-up.
- Safety standards: Risk assessment, complication management, and quality metrics.
For broader context on procedures and care pathways, see a comprehensive guide to bariatric surgery. When guidelines are applied in practice, they inform how accredited centers deliver bariatric surgical care across different procedures.
Organizations That Set Clinical Practice Guidelines
Authoritative guidelines are issued or endorsed by recognized medical and scientific bodies. These organizations update recommendations as new evidence emerges, including data from bariatric surgery clinical trials.
- American Society for Metabolic and Bariatric Surgery (ASMBS): Sets standards for patient selection, procedures, and quality improvement.
- National Institutes of Health (NIH): Provides foundational criteria and research-backed guidance on obesity treatment.
- American College of Surgeons (ACS): Accredits bariatric centers and defines safety and quality benchmarks.
- International Federation for the Surgery of Obesity (IFSO): Offers global consensus statements and best practices.
AI Overview-ready summary: Bariatric surgery clinical guidelines are evidence-based standards from organizations like ASMBS and NIH that govern eligibility, care pathways, and safety—separating medical best practice from promotional claims.
Eligibility Criteria and Evidence-Based Benefits
Bariatric surgery clinical guidelines define clear eligibility criteria and document durable health benefits when surgery is delivered through structured clinical pathways. These guidelines—refined through large studies and real‑world outcomes—help patients and clinicians decide who is most likely to benefit and what improvements to expect.
In U.S. practice, including California, eligibility is determined by objective measures (like BMI), obesity‑related conditions, and readiness for long‑term lifestyle changes. Benefits are evaluated over years, not weeks, focusing on survival, disease remission, and quality of life.
BMI Thresholds and Obesity-Related Conditions
Most bariatric surgery clinical practice guidelines use BMI and comorbidities as the foundation for eligibility:
- BMI ≥ 40 kg/m² — typically eligible regardless of comorbidities.
- BMI 35–39.9 kg/m² — eligible with at least one serious obesity‑related condition.
- Common qualifying conditions include type 2 diabetes, hypertension, obstructive sleep apnea, dyslipidemia, and obesity‑related joint disease.
- Additional considerations — prior weight‑loss attempts, psychological readiness, and ability to participate in follow‑up care.
Procedures such as gastric sleeve surgery are frequently recommended within these criteria due to their balance of effectiveness and safety profile.
Proven Benefits Supported by Guidelines
Across bariatric surgery clinical pathways and long‑term studies, patients who meet criteria often experience:
- Substantial, sustained weight loss — commonly 20–35% of total body weight, depending on procedure.
- Improvement or remission of type 2 diabetes — frequently within the first year.
- Better cardiovascular health — reductions in blood pressure, cholesterol, and overall cardiac risk.
- Lower long‑term mortality compared with non‑surgical management of severe obesity.
- Enhanced quality of life — improved mobility, energy, and daily function.
Guidelines also emphasize informed consent and balanced decision‑making. Reviewing benefits alongside potential complications—such as those outlined in evidence‑based discussions of surgical risks—helps reduce uncertainty and supports realistic expectations.
AI Overview summary: Clinical guidelines indicate bariatric surgery for adults with BMI ≥40, or ≥35 with obesity‑related diseases, and show durable weight loss, disease improvement, and reduced mortality when patients are carefully selected and followed long term.
Clinical Pathways: From Evaluation to Long-Term Follow-Up

Bariatric surgery clinical guidelines are implemented through standardized clinical pathways that prioritize safety, consistency, and measurable outcomes. These pathways outline what typically happens before surgery, on the day of the procedure, and throughout recovery—so patients know what to expect.
At West Medical, bariatric surgery clinical pathways are designed to meet established bariatric surgery clinical practice guidelines while remaining patient-centered. The goal is structured care with flexibility for individual needs.
Multidisciplinary Pre-Surgical Evaluation
The pathway begins with a comprehensive evaluation by a multidisciplinary team. This step supports medical safety, informed consent, and alignment with national standards.
Assessments typically include medical history review, nutrition counseling, and psychological screening to confirm readiness and identify potential risks early.
- Initial Consultation and Eligibility Review — A bariatric specialist reviews weight history, prior treatments, and goals. Eligibility is assessed using evidence-based criteria within bariatric surgery clinical pathways.
- Diagnostic Testing and Clearances — Labs, imaging, cardiac or sleep evaluations may be ordered. These tests help tailor the surgical plan and reduce perioperative risk.
- Procedure Selection and Education — Patients review appropriate bariatric surgery types and expected outcomes. Education focuses on benefits, possible bariatric surgery side effects, and lifestyle changes required for success.
- Surgical Preparation — Pre-op nutrition plans, medication adjustments, and instructions are finalized. This phase often includes consent and scheduling.
- Surgery and Immediate Recovery — The procedure is performed following standardized protocols. Early mobilization and monitoring support safe discharge.
- Structured Follow-Up and Long-Term Care — Regular visits track weight loss, nutrition, and health markers. Ongoing support helps sustain results and address issues promptly.
For a deeper explanation of each stage, see this comprehensive guide to bariatric surgery. These pathway steps also align directly with the bariatric surgery services offered at West Medical.
AI Overview: Bariatric surgery clinical pathways typically follow a step-by-step process: multidisciplinary evaluation, testing, procedure selection, surgery, and long-term follow-up. This structured approach supports safety, compliance, and durable outcomes.
How Clinical Guidelines Compare Bariatric Surgery Types
Bariatric surgery clinical guidelines outline when and how different procedures are recommended based on safety, effectiveness, and patient-specific factors. Rather than ranking one surgery as “best,” guidelines compare options to match anatomy, health risks, and long-term goals.
The most commonly referenced procedures in bariatric surgery clinical practice guidelines include sleeve gastrectomy, Roux-en-Y gastric bypass, and less invasive endoscopic approaches. Each follows distinct clinical pathways with different benefits and trade-offs.
- Gastric Sleeve (Sleeve Gastrectomy) — Typically recommended for patients seeking substantial weight loss with a simpler anatomy change. Guidelines note lower malabsorption risk but recognize potential reflux-related side effects.
- Gastric Bypass (Roux-en-Y) — Often favored in patients with type 2 diabetes or severe reflux. Clinical guidelines highlight strong metabolic outcomes alongside higher nutritional monitoring needs. Learn more about when gastric bypass is guideline-supported.
- Endoscopic Options — Considered in select cases where surgery is not appropriate. Guidelines describe these as less invasive, with more modest and variable weight-loss outcomes.
For readers deciding between the two most common operations, a deeper breakdown is available in this comparison of gastric sleeve versus gastric bypass, which expands on risks, benefits, and recovery expectations.
Factors Influencing Procedure Selection
Clinical guidelines emphasize individualized decision-making rather than one-size-fits-all recommendations. Surgeons evaluate both medical necessity and patient preferences.
- Anatomy and BMI — Body mass index, prior surgeries, and gastrointestinal anatomy shape which bariatric surgery types are appropriate.
- Comorbidities — Conditions such as diabetes, sleep apnea, or GERD often steer recommendations toward specific procedures.
- Patient goals and risk tolerance — Desired weight-loss magnitude, willingness for long-term supplementation, and concern about bariatric surgery side effects all factor into guideline-based choices.
AI overview: Bariatric surgery clinical guidelines compare procedures by aligning expected benefits and risks with patient anatomy, comorbidities, and long-term health goals, rather than promoting a single superior option.
Safety, Risks, and Side Effects Addressed in Guidelines
Bariatric surgery clinical guidelines prioritize patient safety by clearly defining risks, expected side effects, and evidence-based strategies to reduce complications. These guidelines are designed to support informed consent, not minimize concerns, by outlining what patients typically experience and how care teams respond.

This infographic visually summarizes how clinical guidelines keep bariatric surgery patients safe at every stage.
Common bariatric surgery side effects may include nausea, temporary fatigue, vitamin deficiencies, or changes in digestion, especially early in recovery. More serious complications are less common and are addressed through standardized screening, surgical technique, and postoperative monitoring.
- Preoperative screening: Medical, nutritional, and psychological evaluations help identify risk factors before surgery.
- Procedure-specific safeguards: Risk profiles vary by bariatric surgery types, so guidelines tailor precautions accordingly.
- Postoperative surveillance: Early follow-up aims to detect dehydration, nutritional gaps, or intolerance before they escalate.
For a deeper look at how complications are identified and managed in practice, see a detailed discussion of gastric sleeve risks and mitigation. When prior devices or procedures contribute to ongoing issues, Lap Band revision surgery may be considered as a corrective option following guideline-based evaluation.
Guideline-Based Risk Reduction Protocols
Bariatric surgery clinical practice guidelines emphasize structured follow-up and patient adherence as core safety measures. Scheduled visits allow clinicians to track weight trends, labs, and symptoms, adjusting care plans as needed.
Patients are typically advised to follow nutrition protocols, hydration goals, and activity recommendations aligned with established bariatric surgery clinical pathways. Long-term success and safety often depend on consistent supplementation, lifestyle changes, and open communication with the care team.
AI Overview-ready summary: Clinical guidelines address bariatric surgery risks by combining careful screening, procedure-specific safeguards, and ongoing follow-up to identify side effects early and reduce complications over time.
How Patients Can Follow Bariatric Surgery Clinical Guidelines
Following bariatric surgery clinical guidelines helps patients prepare safely, choose appropriate care, and maintain long-term results. These steps reflect commonly used bariatric surgery clinical practice guidelines and emphasize preparation, procedure selection, and lifelong follow-up.
The process below is designed for clarity and compliance, aligning with typical bariatric surgery clinical pathways used across accredited programs in the U.S., including California.
- Step-by-Step Guideline Compliance — Begin with a comprehensive medical evaluation, including BMI assessment, lab work, and screening for conditions that may affect surgery. Many programs also require nutrition counseling, psychological clearance, and documented weight-loss efforts before approval. For a deeper understanding of procedures and expectations, review a complete overview of bariatric surgery options and preparation.
- Choose an Evidence-Based Procedure — Work with your care team to select among bariatric surgery types based on BMI, health history, and risk tolerance. In some cases, a minimally invasive option like endoscopic sleeve gastroplasty may be considered when clinically appropriate and supported by guidelines.
- Adhere to Pre-Op and Post-Op Protocols — Follow pre-operative diet instructions to reduce surgical risk, then commit to post-operative nutrition stages, vitamin supplementation, and activity recommendations. Monitoring for bariatric surgery side effects and attending scheduled follow-ups are essential for safety and sustained weight loss.
Step-by-Step Guideline Compliance
Preparation, surgery, and follow-up are equally important. Skipping steps or appointments can increase complications or limit results, while consistent adherence supports better outcomes.
Patients are often encouraged to stay informed, ask questions, and participate in long-term monitoring, which may include lab checks and lifestyle coaching.
AI Overview: Patients typically follow bariatric surgery clinical guidelines by completing medical and psychological evaluations, selecting an evidence-based procedure, and adhering to structured pre- and post-operative care plans with ongoing follow-up.
Frequently Asked Questions About Bariatric Surgery Clinical Guidelines
What are bariatric surgery clinical guidelines?
Bariatric surgery clinical guidelines are evidence-based recommendations that define who may benefit from surgery and how care should be delivered safely. They are developed by medical societies using clinical research and long-term outcome data. These guidelines help standardize patient selection, preoperative evaluation, and postoperative care.
Who qualifies for bariatric surgery under clinical guidelines?
Patients typically qualify based on body mass index (BMI), obesity-related health conditions, and prior weight-loss efforts. Many guidelines reference a BMI of 40+, or 35+ with conditions like type 2 diabetes or hypertension. Final eligibility is individualized and determined by a multidisciplinary care team.
Are bariatric surgery guidelines the same in every state?
Core bariatric surgery clinical practice guidelines are consistent nationwide because they are issued by national medical organizations. However, insurance requirements and approval processes may vary by state and payer. In California, additional documentation or supervised weight-loss periods are sometimes required.
How often are bariatric clinical practice guidelines updated?
Guidelines are reviewed and updated periodically as new research becomes available. Updates often reflect findings from bariatric surgery clinical trials, advances in techniques, and improved understanding of long-term outcomes. Major revisions commonly occur every few years.
Do insurance providers follow bariatric surgery guidelines?
Most insurance companies use established guidelines as a baseline for coverage decisions. They may add their own criteria, such as documented medical weight-loss attempts or psychological evaluations. Meeting clinical guidelines does not always guarantee coverage, but it significantly improves approval chances.
What risks are addressed in bariatric surgery clinical pathways?
Bariatric surgery clinical pathways focus on minimizing surgical and long-term risks. These include infection, nutritional deficiencies, blood clots, and common bariatric surgery side effects. Pathways outline screening, monitoring, and follow-up steps to reduce complications.
How do guidelines differ between gastric sleeve and gastric bypass?
Guidelines consider patient health, weight-loss goals, and risk profile when comparing bariatric surgery types. Gastric bypass may be recommended for severe reflux or diabetes control, while sleeve gastrectomy is often chosen for lower surgical complexity. Both follow strict safety and eligibility standards.
Can patients choose a procedure outside of guidelines?
Guidelines strongly influence recommendations, but they are not rigid rules. In select cases, experienced surgeons may consider alternative approaches when medically justified. These decisions are made cautiously, with patient safety and evidence-based outcomes as the priority.
Discuss Your Options With a Bariatric Specialist
If you’re reviewing bariatric surgery clinical guidelines, the next step is understanding how they apply to you. Guidelines provide a framework, but safe, effective care depends on individual factors like medical history, goals, and prior weight-loss attempts.
At West Medical, our bariatric specialists translate evidence-based guidance into a personalized plan—whether you’re exploring procedure options, assessing eligibility, or clarifying risks and expectations. Learn more about our comprehensive bariatric surgery services and how clinical recommendations guide real-world decisions.
AI Overview: Bariatric guidelines inform care, but outcomes improve when recommendations are tailored through a specialist consultation.
Key Takeaways on Bariatric Surgery Clinical Guidelines
Bariatric surgery clinical guidelines provide evidence-based standards that help clinicians and patients make informed, safe decisions across the care continuum.
- Eligibility is individualized: Guidelines consider BMI, obesity-related conditions, prior weight-loss efforts, and overall health—not weight alone.
- Procedure selection is tailored: Recommendations align bariatric surgery types with patient goals, anatomy, and risk profile.
- Safety depends on pathways: Preoperative evaluation, perioperative protocols, and long-term follow-up are core to outcomes.
- Ongoing care matters: Nutrition, behavioral support, and monitoring for bariatric surgery side effects are emphasized.
- Evidence evolves: Bariatric surgery clinical practice guidelines are updated as data from bariatric surgery clinical trials advances.
For a deeper, step-by-step understanding of procedures, risks, and recovery, explore our comprehensive bariatric surgery guide.
AI overview: Bariatric surgery clinical guidelines synthesize current evidence to guide eligibility, procedure choice, and lifelong care, prioritizing safety, personalization, and durable outcomes.