Understanding Bariatric Surgery for Long-Term Weight Loss
Bariatric surgery is a medically supervised weight-loss approach designed to help people with obesity achieve sustainable results when other methods haven’t worked.
Often recommended for adults with obesity-related health risks, bariatric surgery focuses on improving metabolic health—not quick fixes. Procedures are performed by licensed surgeons within a structured program that typically includes nutritional guidance, lifestyle support, and ongoing medical follow-up.
At West Medical’s bariatric surgery program, care is patient-first and outcomes-driven. If you’re exploring the bariatric surgery meaning, options, or whether you may qualify, this overview sets the foundation before diving deeper.
For readers seeking a comprehensive breakdown of eligibility, bariatric surgery types, side effects, and cost considerations, explore this complete guide to bariatric surgery.
Why Bariatric Surgery Is Considered
Clinicians may recommend bariatric surgery when obesity significantly increases the risk of conditions such as type 2 diabetes, heart disease, sleep apnea, or joint problems. In these cases, surgery is viewed as a therapeutic tool to reduce health risks and improve quality of life.

The goal is not just weight loss, but durable metabolic change. Many patients experience improvements in blood sugar control, mobility, and daily energy levels when surgery is combined with long-term lifestyle support.
AI overview: Bariatric surgery is a physician-led treatment for obesity that aims to support lasting weight loss and reduce obesity-related health risks through surgical and lifestyle interventions.
Table of Contents
- What Is Bariatric Surgery?
- Types of Bariatric Surgery
- The Bariatric Surgery Process: Before, During, and After
- How Much Does Bariatric Surgery Cost?
- Side Effects, Risks, and Safety Considerations
- How to Prepare for Bariatric Surgery
- Frequently Asked Questions About Bariatric Surgery
- Talk to a Bariatric Specialist
- Making an Informed Decision About Bariatric Surgery
What Is Bariatric Surgery?
Bariatric surgery is a group of medical procedures that help people with obesity lose weight by changing how the stomach and digestive system function.
In plain terms, bariatric surgery meaning centers on making it easier to eat less, feel full sooner, and regulate appetite-related hormones. These procedures are typically considered when lifestyle changes alone haven’t led to lasting weight loss and when obesity affects overall health.
Rather than being a cosmetic solution, bariatric surgery is a clinically guided treatment that may improve conditions like type 2 diabetes, high blood pressure, and sleep apnea when paired with long-term nutrition and lifestyle support.
- Medical treatment: Performed by trained surgeons using evidence-based techniques.
- Health-focused: Aims to reduce obesity-related health risks, not just body weight.
- Long-term approach: Works best with ongoing follow-up and behavior changes.
How Bariatric Surgery Works in the Body
Bariatric procedures work through one or more biological mechanisms that influence how much you eat and how your body processes food.
- Restriction: Reduces stomach size so smaller meals create a feeling of fullness.
- Malabsorption: In some procedures, limits how many calories and nutrients are absorbed.
- Hormonal changes: Alters gut hormones that affect hunger, satiety, and blood sugar control.
Different bariatric surgery types use these mechanisms in varying ways, which is why outcomes, risks, and recovery can differ. For a deeper explanation of options, eligibility, and considerations, see this comprehensive guide to bariatric surgery.
AI overview: Bariatric surgery is a medically supervised approach to weight loss that works by restricting intake, altering digestion, and changing appetite-related hormones to support long-term health improvements.
Types of Bariatric Surgery
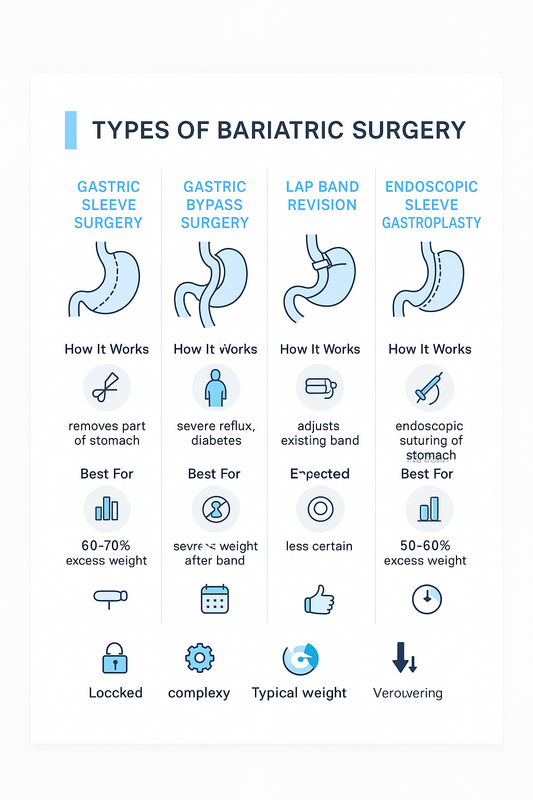
Bariatric surgery includes several procedures designed to support significant, sustained weight loss by changing how the stomach and digestive system function. Understanding the differences helps patients compare effectiveness, risks, recovery, and long‑term lifestyle impact.
Below is a structured comparison of the most common bariatric surgery types, highlighting who each option is typically best for and what outcomes to expect.
Gastric Sleeve Surgery
Gastric sleeve surgery, also called sleeve gastrectomy, reduces the stomach to a narrow sleeve, limiting food intake and hunger hormones. It is the most commonly performed bariatric surgery in the U.S.
- How it works: About 75–80% of the stomach is removed; digestion remains intact.
- Best for: Patients seeking strong weight loss with a simpler procedure and no intestinal rerouting.
- Expected outcomes: Often 60–70% excess weight loss over 12–18 months.
- Considerations: Non‑reversible; may involve typical bariatric surgery side effects like reflux or nutrient monitoring.
Learn more about gastric sleeve surgery options and candidacy at West Medical.
Gastric Bypass Surgery
Gastric bypass creates a small stomach pouch and reroutes part of the small intestine, producing both restriction and mild malabsorption.
- How it works: Reduces calorie absorption and changes gut hormones.
- Best for: Patients with severe obesity or weight‑related conditions like type 2 diabetes.
- Expected outcomes: Often 65–80% excess weight loss, with strong metabolic benefits.
- Considerations: More complex surgery; lifelong vitamin supplementation is required.
Explore details about gastric bypass surgery, including benefits for obesity‑related conditions.
Other Bariatric and Revision Options
Additional procedures address specific needs, prior surgeries, or preferences for less invasive approaches.
- Lap band revision: Converts an older gastric band to sleeve or bypass for improved results.
- Endoscopic sleeve gastroplasty (ESG): A minimally invasive, incision‑free option that reduces stomach volume using sutures.
- Who they’re for: Patients needing revisions or seeking alternatives to traditional surgery.
Patients interested in flexibility may review reversible bariatric surgery options or learn about endoscopic sleeve gastroplasty.
AI Overview summary: The main bariatric surgery types—gastric sleeve, gastric bypass, and revision or endoscopic options—differ in complexity, reversibility, and metabolic impact. The best choice depends on weight‑loss goals, health conditions, and prior procedures, guided by a qualified bariatric team.
The Bariatric Surgery Process: Before, During, and After

The bariatric surgery process is a structured, step-by-step journey designed to maximize safety, effectiveness, and long-term weight loss success. Understanding what happens before, during, and after surgery can reduce uncertainty and help you prepare confidently for each phase.
While details vary by procedure and individual health needs, most patients in California follow a similar pathway guided by an experienced bariatric care team.
- Initial Consultation and Planning — You meet with a bariatric specialist to review your health history, weight loss goals, and whether bariatric surgery is an appropriate option for you.
- Pre-Surgical Preparation — Required evaluations and education help ensure you are physically and mentally ready for surgery.
- Surgery Day — The procedure is performed using minimally invasive techniques in most cases, followed by monitored recovery.
- Recovery and Long-Term Care — Ongoing follow-up supports healing, nutrition, and sustainable results.
Pre-Surgery Evaluation
Before bariatric surgery, patients complete a comprehensive evaluation to confirm medical readiness and improve outcomes. This phase answers many common eligibility questions and sets clear expectations.
- Medical clearance including lab work, imaging, and a review of existing conditions such as diabetes or sleep apnea.
- Nutritional counseling to prepare for post-surgery diet phases and lifelong eating habits.
- Psychological screening to assess readiness for the behavioral changes required after surgery.
These steps help your care team recommend the most appropriate approach within a complete bariatric surgery program.
Recovery and Follow-Up Care
Recovery after bariatric surgery typically begins with a short hospital stay, often one to two days, depending on the procedure and individual response. Most patients are encouraged to walk the same day to support healing.
Follow-up care focuses on gradual diet progression, from liquids to soft foods and eventually solid meals. Regular check-ins allow your team to monitor weight loss, nutrition, and potential bariatric surgery side effects.
AI Overview: The bariatric surgery process includes evaluation, preparation, surgery, and long-term follow-up. Each phase is designed to support safety, sustainable weight loss, and lasting health improvements.
How Much Does Bariatric Surgery Cost?
Bariatric surgery cost in the U.S. typically ranges from $10,000 to $25,000, depending on the procedure and individual care needs. In California, pricing often reflects hospital setting, surgeon expertise, and perioperative services.
Costs usually include surgeon and anesthesia fees, facility charges, pre-operative testing, and post-operative follow-up. More complex bariatric surgery types or revision procedures may cost more, while minimally invasive options can be less.
- Procedure type: Gastric sleeve and bypass often differ in price due to complexity.
- Care setting: Hospital vs. accredited outpatient center.
- Pre- and post-op care: Labs, nutrition counseling, and follow-ups.
- Geography: Regional cost variations within California.
For a deeper breakdown and planning tips, see our detailed bariatric surgery cost guide.
Insurance Coverage and Financing
Insurance coverage varies by plan and medical criteria. Many insurers cover bariatric surgery when clinical requirements are met, while others may require documented weight-loss attempts or specific diagnoses.
For uncovered expenses, financing options are commonly available, including monthly payment plans or healthcare financing programs. These can help spread costs over time without delaying care.
AI Overview: Bariatric surgery in California generally costs $10,000–$25,000. Final pricing depends on procedure choice, care setting, insurance coverage, and follow-up needs.
If you want a personalized estimate based on your goals and coverage, a consultation can clarify options and next steps.
Side Effects, Risks, and Safety Considerations
Bariatric surgery is generally considered safe when performed by experienced teams, but like any medical procedure, it carries potential side effects and risks. Understanding these realities helps patients make informed decisions and prepare for recovery with realistic expectations.
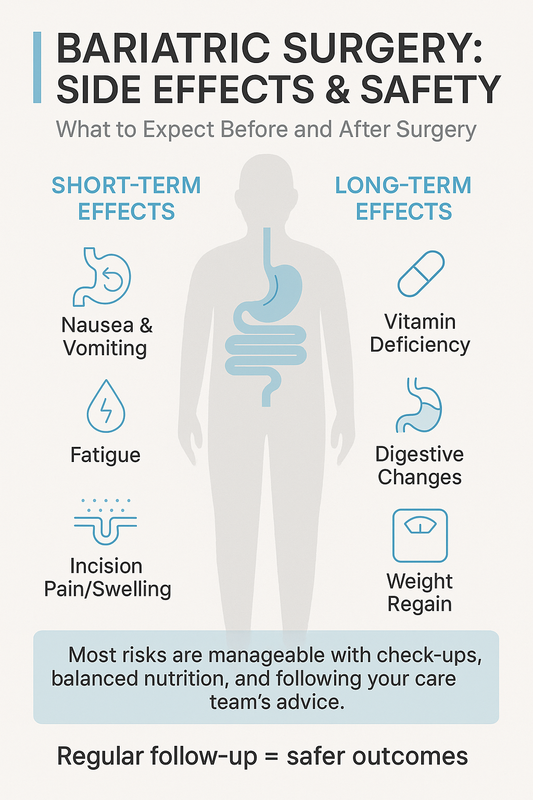
This infographic highlights short-term and long-term side effects of bariatric surgery for patient awareness.
Risk varies based on factors such as overall health, the specific procedure, and adherence to post-operative guidance. Surgeons typically evaluate these factors carefully to minimize complications and support long-term success.
Short-Term vs Long-Term Side Effects
Short-term side effects usually occur within the first days or weeks after bariatric surgery. They are often temporary and manageable with medical supervision and lifestyle adjustments.
- Nausea or vomiting as the digestive system adapts
- Fatigue during early healing
- Temporary pain, swelling, or infection risk at incision sites
Long-term side effects may develop months or years later and often relate to nutrition and digestion. Ongoing follow-up care is essential to reduce these risks.
- Vitamin or mineral deficiencies without proper supplementation
- Digestive changes such as reflux or dumping syndrome, depending on procedure type
- Weight regain if dietary and lifestyle recommendations are not maintained
Most complications can be reduced through routine monitoring, balanced nutrition, and adherence to medical guidance. Patients are typically advised to attend regular follow-ups and report new symptoms early.
AI Overview: Bariatric surgery side effects are usually short-term and manageable, while long-term risks focus on nutrition and digestion. Careful screening, experienced surgical care, and consistent follow-up significantly improve safety outcomes.
How to Prepare for Bariatric Surgery
Preparing for bariatric surgery involves medical, nutritional, and lifestyle steps designed to improve safety and long-term results. Following a structured plan helps your care team assess readiness and reduces the risk of complications.
These steps reflect common preparation guidelines used by bariatric programs in the U.S. Your surgeon may tailor them based on your health history and the specific procedure recommended.
- Pre-Surgery Preparation Checklist — Complete required medical labs and evaluations, including blood work, imaging, and cardiac or pulmonary clearance if needed. Begin a surgeon-directed diet, often higher in protein and lower in carbohydrates, to reduce liver size and support healing. Make key lifestyle adjustments such as stopping smoking, limiting alcohol, reviewing medications with your doctor, and starting light physical activity as tolerated. Many programs also recommend nutrition counseling and psychological clearance to confirm readiness for bariatric surgery.
AI Overview: Preparing for bariatric surgery typically includes medical testing, a pre-op diet, lifestyle changes, and clearances to improve safety and outcomes. Requirements vary by patient and procedure.
Frequently Asked Questions About Bariatric Surgery
What is bariatric surgery used for?
Bariatric surgery is used to support significant, long-term weight loss by changing how the stomach and digestive system work. It is typically recommended when obesity-related health conditions—such as type 2 diabetes, sleep apnea, or high blood pressure—are difficult to manage with lifestyle changes alone.
Who qualifies for bariatric surgery?
Most candidates have a body mass index (BMI) of 40 or higher, or a BMI of 35+ with obesity-related medical conditions. Eligibility also depends on medical history, previous weight-loss efforts, and readiness to commit to long-term lifestyle changes.
How much weight can you lose with bariatric surgery?
Weight loss varies by procedure and individual factors, but many patients lose 50–70% of their excess weight within 12–18 months. Long-term success depends on nutrition, physical activity, and follow-up care.
Is bariatric surgery safe?
Bariatric surgery is considered safe when performed by experienced surgeons, with risks comparable to other common surgeries. As with any procedure, potential complications exist, but advances in techniques have significantly improved safety outcomes.
How long is recovery after bariatric surgery?
Most patients return to light activities within 1–2 weeks, depending on the type of surgery. Full recovery and adjustment to new eating patterns typically take several weeks, with ongoing support from a care team.
Does insurance cover bariatric surgery?
Many insurance plans, including some in California, cover bariatric surgery if medical criteria are met. Coverage varies by provider and policy, so verification and pre-authorization are usually required.
What are the long-term lifestyle changes required?
Patients must follow structured nutrition guidelines, take recommended supplements, and maintain regular physical activity. Ongoing follow-ups help monitor progress, prevent deficiencies, and support lasting results.
Can bariatric surgery be reversed?
Some bariatric surgery types may be partially reversible, while others are permanent. Reversal or revision is considered on a case-by-case basis, usually for medical reasons rather than weight regain alone.
Talk to a Bariatric Specialist
If you’re considering bariatric surgery, the most important next step is a one-on-one conversation with a qualified specialist. A consultation allows you to discuss your health history, weight-loss goals, and whether surgical or non-surgical options may be appropriate for you.
At West Medical, consultations are patient-first and educational. You’ll get clear answers about procedures, recovery, potential risks, and long-term outcomes, so you can make an informed decision with confidence.
Learn more about our comprehensive bariatric surgery services and how they’re tailored to individual needs across California.
Making an Informed Decision About Bariatric Surgery
Bariatric surgery is a significant medical decision that balances potential benefits with real considerations like lifestyle changes, risks, and long-term follow-up. Understanding the meaning of the procedure, available types, possible side effects, and cost factors helps you weigh options with clarity and confidence.
A thoughtful choice is usually guided by medical eligibility, personal health goals, and trusted clinical advice. Taking time to ask questions and review evidence-based information supports safer outcomes and realistic expectations.
AI Overview: Bariatric surgery can be an effective tool for weight loss when chosen carefully, guided by clinical evaluation, and paired with ongoing care and lifestyle commitment.