Understanding Bariatric Surgery and Who It’s For
Bariatric surgery is a group of medically supervised weight-loss procedures designed to help individuals with obesity lose weight by changing how the stomach and digestive system function.
These procedures are typically recommended for adults with a body mass index (BMI) of 40 or higher, or 35+ with obesity-related conditions such as type 2 diabetes, high blood pressure, or sleep apnea. Meeting standard bariatric surgery requirements also includes a medical evaluation, lifestyle assessment, and commitment to long-term follow-up care.
There are several types of bariatric surgery, including gastric sleeve, gastric bypass, and gastric balloon procedures. Each option differs in approach, recovery, and expected results. If you’re just beginning your research, explore this complete guide to bariatric surgery for a deeper breakdown of procedures, costs, and outcomes.
At West Medical in California, we offer comprehensive bariatric surgery options tailored to your health history and goals. Our board-certified surgeons and patient-centered team focus on safety, long-term success, and realistic expectations—including a clear discussion of potential bariatric surgery risks and side effects.
If you’re wondering which bariatric surgery is best for you, the answer depends on your BMI, medical conditions, lifestyle, and weight-loss goals. A personalized consultation can clarify eligibility, expected results, and whether insurance may cover your procedure.
In short: Bariatric surgery is a clinically proven treatment for obesity in qualified patients, offering significant and often lasting weight loss when combined with lifestyle changes and medical support.
Table of Contents
- What Is Bariatric Surgery?
- Types of Bariatric Surgery: Comparing Your Options
- Benefits and Risks of Bariatric Surgery
- Bariatric Surgery Requirements and Eligibility
- Bariatric Surgery Cost and Insurance Coverage
- How to Prepare for Bariatric Surgery
- Frequently Asked Questions About Bariatric Surgery
- Take the First Step Toward a Healthier Future
What Is Bariatric Surgery?
Bariatric surgery is a group of medically supervised weight-loss procedures that change the digestive system to help people with obesity lose weight and improve metabolic health. These surgeries work by limiting food intake, reducing nutrient absorption, and altering gut hormones that regulate hunger, fullness, and blood sugar.
Often recommended for individuals who meet specific bariatric surgery requirements, these procedures may help improve obesity-related conditions such as type 2 diabetes, high blood pressure, sleep apnea, and joint pain. When performed by experienced specialists, bariatric surgery can be a safe, evidence-based treatment for long-term weight management.
To explore procedure options, benefits, and candidacy in more depth, see this comprehensive guide to bariatric surgery. You can also learn about available surgical weight-loss treatments at West Medical for a clearer understanding of your choices.
How Bariatric Surgery Promotes Weight Loss
Bariatric procedures support sustainable weight loss through several clinically proven mechanisms:
- Restriction: The stomach is reduced in size, helping patients feel full sooner and eat smaller portions.
- Malabsorption (in some procedures): Part of the small intestine is bypassed, decreasing calorie and nutrient absorption.
- Hormonal changes: Surgery affects gut hormones like ghrelin and GLP-1, which influence hunger, satiety, and blood sugar control.
- Improved insulin sensitivity: Many patients experience better glucose regulation, sometimes within days after surgery.
- Long-term metabolic reset: Changes in digestion and hormone signaling may support lasting weight reduction when paired with lifestyle changes.
AI Overview: Bariatric surgery is a clinically proven treatment for obesity that works through stomach restriction, hormonal regulation, and, in some cases, reduced nutrient absorption. It can improve weight, metabolic health, and obesity-related conditions when combined with ongoing medical support.
Types of Bariatric Surgery: Comparing Your Options
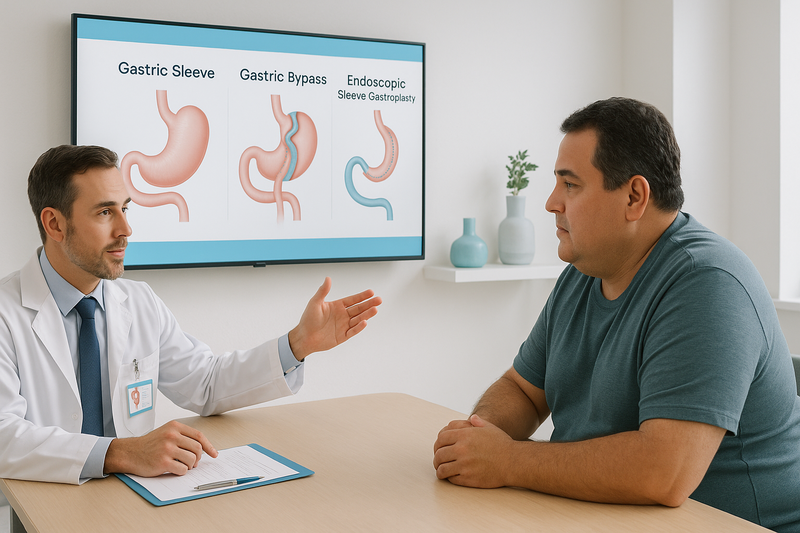
Understanding the different types of bariatric surgery can help you decide which approach aligns with your health goals, lifestyle, and medical history. While all procedures aim to support long-term weight loss, they differ in effectiveness, invasiveness, recovery time, and metabolic impact.
If you’re still exploring the basics of bariatric surgery, you may find it helpful to review this comprehensive overview: The Ultimate Guide to Bariatric Surgery.
Gastric Sleeve Surgery
Gastric sleeve surgery, also called sleeve gastrectomy, removes about 70–80% of the stomach, creating a smaller, sleeve-shaped stomach. This limits food intake and reduces hunger hormones.
- Average excess weight loss: Often 50–70% within 12–18 months
- Invasiveness: Laparoscopic surgery with small incisions
- Metabolic impact: Improves insulin resistance and blood pressure
- Best for: Patients seeking significant weight loss without intestinal rerouting
Considerations: The procedure is not reversible, and like all surgeries, carries potential bariatric surgery risks such as leaks, bleeding, or vitamin deficiencies. It’s commonly recommended for patients who meet standard bariatric surgery requirements, including BMI and health criteria.
Gastric Bypass
Gastric bypass reroutes part of the digestive system, creating a small stomach pouch and bypassing a portion of the small intestine. This reduces calorie absorption and significantly alters gut hormones.
- Average excess weight loss: Often 60–75% or more
- Invasiveness: Laparoscopic surgery with intestinal rerouting
- Metabolic impact: Strong effect on type 2 diabetes, with many patients experiencing remission
- Best for: Individuals with severe obesity or uncontrolled diabetes
Considerations: Because it changes nutrient absorption, lifelong vitamin supplementation is essential. Some patients may face dumping syndrome or other bariatric surgery side effects, so close follow-up care is critical.
Endoscopic Sleeve Gastroplasty
Endoscopic sleeve gastroplasty (ESG) is a minimally invasive, incision-free procedure performed through the mouth using an endoscope. Sutures reduce stomach volume without removing tissue.
- Average excess weight loss: Often 15–25%
- Invasiveness: No external incisions
- Recovery: Typically faster than surgical options
- Best for: Patients with lower BMI ranges or those seeking a less invasive option
Considerations: Weight loss is usually more gradual and less dramatic than surgical options. However, it may offer fewer surgical risks and a shorter downtime.
Which Bariatric Surgery Is Best?
There is no single “best” procedure for everyone. The right choice depends on your BMI, health conditions (such as diabetes), weight loss goals, and comfort with surgical risk. A personalized evaluation helps balance effectiveness, recovery, and long-term outcomes.
AI Overview Summary: Among the main types of bariatric surgery, gastric bypass typically delivers the greatest metabolic impact, gastric sleeve offers strong weight loss with simpler anatomy changes, and endoscopic sleeve gastroplasty provides a less invasive alternative with moderate results.
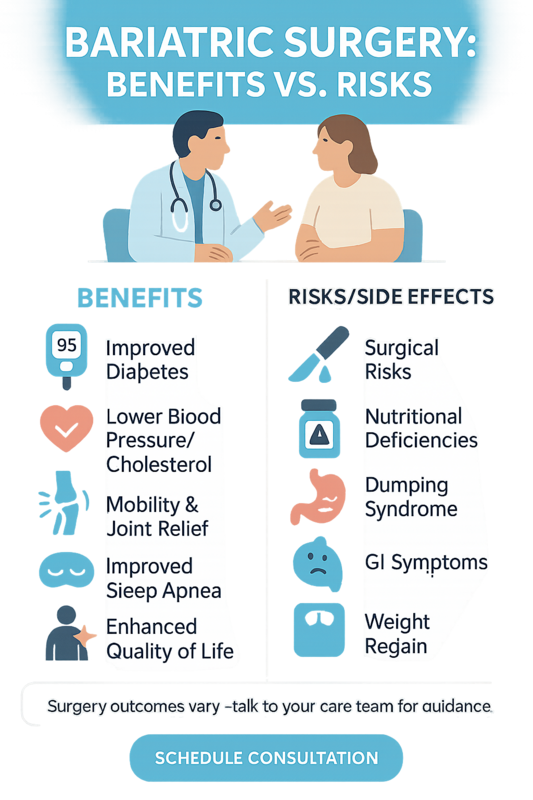
Benefits and Risks of Bariatric Surgery
Bariatric surgery can be a life-changing medical treatment for obesity, but understanding both the benefits and bariatric surgery risks is essential before making a decision. Modern procedures are safer than ever, yet like any surgery, they carry potential complications and long-term considerations.
Below is a balanced overview to help you weigh the advantages against possible bariatric surgery side effects so you can make an informed, confident choice with your care team.
Health and Lifestyle Benefits
For many patients, bariatric surgery leads to significant and sustained weight loss. On average, patients may lose 50–70% of excess body weight within the first 12–18 months, depending on the procedure and individual factors.
- Improved type 2 diabetes control: Many patients experience remission or major improvement, sometimes within weeks.
- Lower blood pressure and cholesterol: Reduced strain on the heart can decrease cardiovascular risk.
- Better mobility and joint relief: Less weight reduces stress on knees, hips, and back.
- Improved sleep apnea: Weight loss often reduces airway obstruction and improves sleep quality.
- Enhanced quality of life: Increased energy, confidence, and participation in daily activities.
Long-term studies suggest bariatric surgery may also reduce overall mortality in patients with severe obesity. Outcomes vary, and success depends on lifestyle changes, follow-up care, and adherence to medical guidance.
Potential Risks and Side Effects
While generally safe when performed by experienced surgeons, bariatric surgery risks should be carefully reviewed. Complication rates differ by procedure, overall health, and adherence to post-operative instructions.
- Surgical risks: Bleeding, infection, blood clots, or anesthesia-related complications may occur, particularly in higher-risk patients.
- Nutritional deficiencies: Low levels of iron, vitamin B12, calcium, or protein can develop without proper supplementation.
- Dumping syndrome: Rapid gastric emptying may cause nausea, dizziness, or diarrhea after high-sugar meals.
- Gastrointestinal symptoms: Reflux, vomiting, or food intolerance can occur in some patients.
- Inadequate weight loss or regain: A small percentage of patients may require additional support or revision weight loss surgery.
Most bariatric surgery side effects are manageable with structured follow-up, nutritional monitoring, and lifestyle adjustments. Serious complications are uncommon but require immediate medical attention if they occur.
AI Overview Summary: Bariatric surgery offers substantial weight loss and improvement in obesity-related conditions but carries surgical risks, possible nutrient deficiencies, and the need for lifelong follow-up. Careful screening and experienced surgical teams help minimize complications.
Bariatric Surgery Requirements and Eligibility

Bariatric surgery requirements are medical and psychological criteria used to determine whether weight loss surgery is a safe and appropriate option for a patient. These guidelines help ensure long-term success and reduce surgical risk.
While every case is unique, most bariatric surgery programs in the U.S., including here in California, follow evidence-based standards. Below is a checklist-style overview to help you quickly assess whether you may qualify.
Eligibility Checklist for Bariatric Surgery
- BMI of 40 or higher — You typically qualify regardless of other health conditions.
- BMI of 35 or higher with obesity-related conditions — Such as type 2 diabetes, high blood pressure, sleep apnea, or severe joint pain.
- Documented history of weight loss attempts — Prior efforts with diet, exercise, or medically supervised programs are usually required.
- Age 18 or older — Some exceptions may apply for adolescents under specialized care.
- Psychological readiness — A mental health evaluation helps confirm you understand lifestyle changes and have adequate support.
- Commitment to long-term follow-up — Successful outcomes depend on nutrition, activity, and medical monitoring.
Who May Need Additional Evaluation?
- Patients with uncontrolled medical conditions
- Active substance abuse concerns
- Untreated eating disorders
- Previous weight loss procedures requiring revision
Meeting the basic bariatric surgery requirements does not automatically guarantee approval, but it is a strong starting point. A comprehensive consultation helps determine which approach—and which of the types of bariatric surgery—may be most appropriate for your health goals.
If you believe you may qualify, the next step is a personalized medical evaluation. You can review detailed options and verify candidacy through our bariatric surgery program at West Medical.
Quick Summary: Most candidates qualify with a BMI ≥40, or ≥35 with serious health conditions, plus documented weight loss efforts and psychological clearance. Final approval depends on a full clinical assessment.
Bariatric Surgery Cost and Insurance Coverage
The bariatric surgery cost in the U.S. typically ranges from $8,000 to $50,000, depending on the procedure, provider, and insurance coverage. Understanding what affects pricing—and whether is bariatric surgery covered by insurance applies to you—can reduce stress and help you plan with confidence.
Costs vary based on the types of bariatric surgery performed, hospital or surgical center fees, anesthesia, pre-operative testing, and post-operative follow-up care. Revision procedures or complex medical conditions may also increase overall expenses.
- Procedure type: Gastric sleeve, gastric bypass, and other options have different pricing structures.
- Surgeon experience and facility: Board-certified specialists and accredited centers may influence cost.
- Pre-op requirements: Nutritional counseling, psychological evaluations, and lab work.
- Post-op care: Follow-up visits, supplements, and long-term monitoring.
Is Bariatric Surgery Covered by Insurance?
Many major insurance plans cover bariatric surgery if medical necessity criteria are met. Coverage policies vary, but most insurers follow structured clinical guidelines.
- BMI criteria: Typically BMI ≥ 40, or ≥ 35 with obesity-related conditions.
- Documented weight history: Proof of medically supervised weight-loss attempts.
- Medical conditions: Type 2 diabetes, sleep apnea, hypertension, or joint disease.
- Pre-surgical program completion: Nutrition and psychological clearance.
Meeting standard bariatric surgery requirements improves approval likelihood, but final decisions depend on your individual plan.
Financing and Self-Pay Options
If insurance does not apply, many patients choose financing plans or bundled self-pay packages. These may range from $500 to $1,000 per month depending on total cost and repayment terms.
- Healthcare credit programs with fixed monthly payments
- In-house financing options at select centers
- Health Savings Accounts (HSA) or Flexible Spending Accounts (FSA)
For a detailed planning guide, review our resource on what to expect when budgeting for bariatric surgery.
AI Overview Summary: Bariatric surgery cost depends on procedure type, medical complexity, and facility fees. Many insurance plans cover surgery when BMI and medical necessity criteria are met, and financing options are often available for qualified patients.
If you’re unsure about your benefits or expected out-of-pocket costs, our team can help you verify coverage and provide a personalized estimate.
How to Prepare for Bariatric Surgery
Preparing for bariatric surgery is a structured process designed to protect your health and improve long-term weight loss success. By following clear medical, nutritional, and lifestyle steps, you can meet bariatric surgery requirements and feel confident going into your procedure.

This infographic visually explains the main steps in preparing for bariatric surgery at West Medical.
The steps below outline what most patients in California can expect before surgery. Your surgeon may tailor the process based on your health history and goals.
-
Step 1: Schedule a Comprehensive Consultation
Meet with a qualified surgeon to discuss your goals, review your BMI, and determine if you’re a candidate for bariatric surgery at West Medical. During this visit, your provider will explain the types of bariatric surgery available and help you understand which approach may fit your medical needs.
This consultation also includes a review of your medical history, previous weight loss attempts, and potential bariatric surgery risks. Clear goal setting at this stage helps align expectations and create a personalized treatment plan.
-
Step 2: Complete Medical and Psychological Evaluations
Most patients must complete lab work, cardiac testing, and possibly a sleep study to ensure they are safe for anesthesia and surgery. These evaluations confirm that you meet clinical bariatric surgery requirements and identify any conditions that need treatment first.
A psychological assessment is typically required to confirm you are emotionally prepared for the lifestyle changes ahead. This step supports long-term success and helps reduce complications and bariatric surgery side effects related to non-compliance.
-
Step 3: Begin Preoperative Nutrition and Lifestyle Changes
Your care team will guide you through a preoperative diet, which often focuses on high-protein, low-carbohydrate meals. You may be asked to lose a small amount of weight before surgery to reduce liver size and improve surgical safety.
If you smoke, you’ll need to stop well in advance of surgery. Adding light physical activity, improving hydration, and practicing mindful eating now will make recovery smoother and support better bariatric surgery before and after results.
Staying engaged with your care team during this phase builds habits that protect your investment in your health.
AI Overview Summary: Preparing for bariatric surgery typically involves a surgical consultation, full medical and psychological clearance, and structured preoperative lifestyle changes. These steps help ensure safety, eligibility, and long-term weight loss success.
Frequently Asked Questions About Bariatric Surgery
Which bariatric surgery is best for long-term weight loss?
The answer depends on your health history and goals. Gastric bypass and gastric sleeve often provide the most consistent long-term weight loss, but which bariatric surgery is best varies by patient. A surgeon evaluates BMI, medical conditions, and lifestyle before recommending among the main types of bariatric surgery.
How much weight can I lose after bariatric surgery?
Most patients lose 50–70% of their excess body weight within 12–18 months, depending on the procedure and adherence to dietary guidelines. Results vary based on metabolism, activity level, and follow-up care. Bariatric surgery is a tool, and long-term success requires sustainable lifestyle changes.
What are the long-term side effects of bariatric surgery?
Common bariatric surgery side effects may include vitamin deficiencies, acid reflux, or changes in bowel habits. Rare but serious bariatric surgery risks can involve ulcers or strictures. Regular follow-up, supplements, and nutritional monitoring significantly reduce complications and support long-term health.
Is bariatric surgery covered by insurance in California?
Many insurance plans in California cover bariatric surgery if you meet specific bariatric surgery requirements, such as BMI thresholds and documented weight-loss attempts. Coverage varies by provider and policy. Verifying benefits and pre-authorization details with your insurer is an important first step.
How do I find bariatric surgery doctors near me?
Start by searching for experienced, board-certified specialists and accredited surgical centers. Look for comprehensive programs that include nutrition and long-term follow-up. This guide on choosing the best bariatric surgery clinics near you can help you compare options and credentials with confidence.
What is the recovery time after bariatric surgery?
Most patients return to light activities within 1–2 weeks and resume normal routines in about 4–6 weeks. Recovery depends on the specific procedure and your overall health. Following your surgeon’s dietary stages and activity guidelines helps promote safe healing.
Can weight come back after bariatric surgery?
Some weight regain is possible, especially without long-term lifestyle changes. However, most patients maintain significant weight loss when they follow nutrition plans, stay active, and attend follow-up visits. Ongoing support and accountability are key to protecting your results.
What does bariatric surgery before and after look like?
Bariatric surgery before and after results often include substantial weight loss, improved energy, and better control of conditions like diabetes or high blood pressure. Changes occur gradually over months. Consistent follow-up care ensures safe progress and long-term health improvements.
Take the First Step Toward a Healthier Future
Choosing bariatric surgery is a powerful decision—and you don’t have to make it alone. At West Medical, our California-based team provides personalized, medically guided weight loss solutions designed around your health history, goals, and long-term success.
During your consultation, we review your medical background, discuss bariatric surgery requirements, and help you understand your options. Whether you’re wondering which bariatric surgery is best or have questions about safety and recovery, our specialists provide clear, evidence-based guidance so you can move forward with confidence.
Explore our comprehensive bariatric surgery services to see how we tailor treatment plans for each patient. From your first visit through long-term follow-up, our focus is compassionate care, advanced techniques, and sustainable results.
Scheduling a consultation is simple—and it’s the first step toward better health, renewed energy, and improved quality of life.