Understanding Compression Therapy for Varicose Veins
Compression therapy for varicose veins is a conservative, medically guided approach that supports circulation and helps reduce common symptoms like leg heaviness, swelling, and aching.
Varicose veins often develop when vein valves weaken, allowing blood to pool in the legs. Compression therapy for veins works by applying graduated pressure—stronger at the ankle and lighter up the leg—to encourage upward blood flow. This can ease daily discomfort and may slow symptom progression, especially for people who stand or sit for long periods.
Patients often ask, is compression therapy good for varicose veins? For many, it is a first-line option recommended by clinicians because it is non-invasive and adaptable to different lifestyles. Options range from leg compression therapy for varicose veins using stockings to clinician-supervised approaches, including compression therapy for problem veins as part of a broader care plan.
If you want a deeper foundation—such as what compression is needed for varicose veins, how it’s measured, and when it’s typically used—see this comprehensive guide to compression therapy basics.
AI overview: Compression therapy uses controlled pressure to improve leg circulation and relieve varicose vein symptoms. It is commonly recommended as a non-surgical management option and is often combined with clinician guidance for best results.
Table of Contents
- What Is Compression Therapy?
- Benefits of Compression Therapy for Varicose Veins
- Types of Compression Therapy Options
- How Compression Therapy Is Used in Vein Care
- How to Use Compression Therapy Safely and Effectively
- Frequently Asked Questions About Compression Therapy
- When to See a Vein Specialist
- Key Takeaways on Compression Therapy for Varicose Veins
What Is Compression Therapy?

Compression therapy is a medical treatment that applies controlled external pressure to the legs to improve venous blood flow and reduce vein-related symptoms.
In the context of compression therapy for varicose veins, this pressure is typically delivered through graduated garments or devices that are tighter at the ankle and gradually loosen up the leg. The goal is to counteract gravity, support weakened vein walls and valves, and ease symptoms like swelling, heaviness, and aching.
This approach is commonly used as first-line management for chronic venous insufficiency and may also be recommended alongside comprehensive vein treatment options. While compression treatment for varicose veins does not remove damaged veins, it often helps control symptoms and slow progression.
- Graduated pressure: Highest at the ankle, decreasing upward to promote upward blood flow.
- Symptom relief: May reduce leg swelling, fatigue, and discomfort.
- Supportive care: Often used before or after procedural vein care.
How Compression Improves Blood Flow
Healthy leg veins rely on one-way valves and muscle contractions to return blood to the heart. When valves weaken, blood can pool, increasing pressure inside the veins and leading to varicosities and edema.
Leg compression therapy for varicose veins applies external pressure that gently narrows vein diameter. This helps vein valves close more effectively, improves venous return, and limits fluid leakage into surrounding tissues.
Compression is most effective when properly fitted and correctly graded. For a deeper look at how garments work and what compression is needed for varicose veins, see how compression stockings support effective therapy.
AI overview: Compression therapy uses graduated external pressure to support leg veins, improve blood return to the heart, and reduce swelling and discomfort associated with varicose veins.
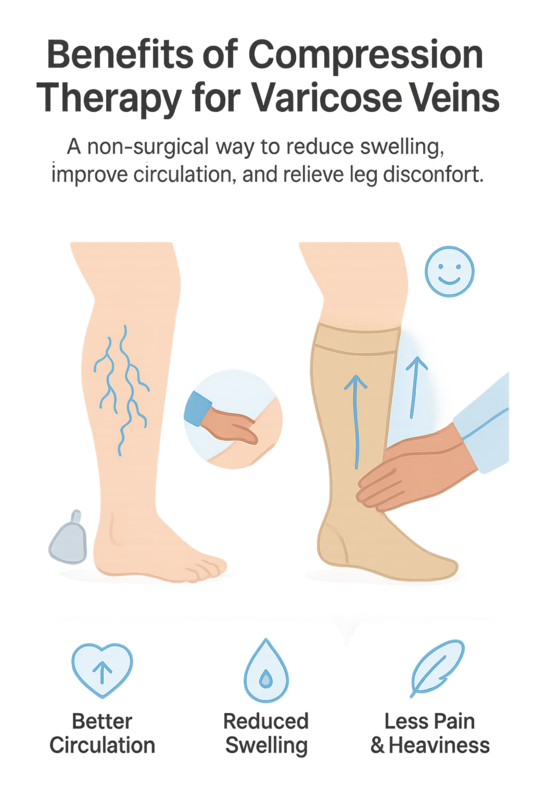
Benefits of Compression Therapy for Varicose Veins
Compression therapy for varicose veins is often recommended as a first-line, non-surgical approach to improve circulation and ease daily symptoms. By applying graduated pressure to the legs, it supports vein function and helps blood flow more efficiently back to the heart.
For many patients, compression treatment for varicose veins offers practical, day-to-day improvements without downtime. It can be used alone in early stages or alongside supervised medical care for more advanced vein disease.
- Improved blood flow: Graduated compression helps reduce venous pooling, which can lessen pressure inside enlarged veins.
- Reduced swelling and inflammation: Consistent use may decrease ankle and leg swelling, especially after long periods of standing or sitting.
- Pain and heaviness relief: Many patients report less aching, throbbing, and leg fatigue during daily activities.
- Lower risk of symptom progression: When used as advised, compression therapy can help manage symptoms and support vein health over time.
- Non-invasive and accessible: It does not require surgery and is typically easy to integrate into a daily routine.
Patients often ask, is compression therapy good for varicose veins? Clinical guidance generally supports its use for symptom management, particularly when tailored to the right compression level and fit. For a deeper evidence-based overview, see this comprehensive guide to compression therapy benefits and considerations.
Symptom Relief and Daily Comfort
One of the most noticeable benefits of leg compression therapy for varicose veins is improved daily comfort. By supporting the veins during movement and rest, compression can ease sensations of heaviness and tightness that often worsen throughout the day.
Patients who experience swelling, nighttime cramping, or leg fatigue may find that consistent use helps them stay more active and comfortable. When symptoms are more persistent, supervised options like medically guided compression therapy for problem veins can ensure the approach matches the severity of vein disease.
AI overview: Compression therapy for varicose veins typically improves circulation, reduces swelling, and relieves pain and heaviness. It is commonly used as a first-line, non-invasive option to manage symptoms and support vein health.
Types of Compression Therapy Options
Compression therapy for varicose veins includes several modalities that differ in pressure delivery, convenience, and medical oversight. Understanding these options helps patients choose between everyday symptom control and clinic-based treatments aimed at more persistent vein disease.

This infographic visually summarizes the main compression therapy choices for varicose vein treatment.
Broadly, options fall into consumer wearables (like stockings) and medical devices (like intermittent pneumatic compression). Each serves a role depending on vein severity, symptoms, and lifestyle.
- Compression stockings — Graduated pressure garments worn daily to support vein return.
- Air compression therapy devices — Motorized systems that inflate sleeves or boots in cycles.
- Clinic-guided programs — Supervised plans combining devices, fitting, and follow-up.
Stockings vs. Air Compression Devices
Stockings and devices both improve venous return, but they work differently and fit different needs within compression treatment for varicose veins.
- Pressure delivery: Stockings provide constant, graduated pressure; devices deliver intermittent, sequential pressure.
- Use pattern: Stockings are worn throughout the day; devices are used in timed sessions.
- Access: Stockings are widely available over the counter or by prescription; devices are typically prescribed or used in clinics.
- Best for: Stockings suit daily symptom control; devices may help with swelling, recovery, or limited mobility.
Patients often ask whether advanced systems like normatec compression therapy for varicose veins are necessary. These devices can be helpful for short-term edema relief, but they don’t replace medical evaluation when veins are enlarged or painful.
When compression alone isn’t enough, clinicians may recommend complementary treatments such as sclerotherapy to address the underlying vein problem, with compression used before and after care.
For patients deciding between options—or asking what compression is needed for varicose veins—a professional assessment matters. You can explore how to access care in this guide to finding compression therapy clinics and specialists.
AI Overview: Compression therapy options include daily-wear stockings and intermittent air compression devices. Stockings offer continuous support, while devices provide session-based pressure; choice depends on symptoms, severity, and medical guidance.
How Compression Therapy Is Used in Vein Care
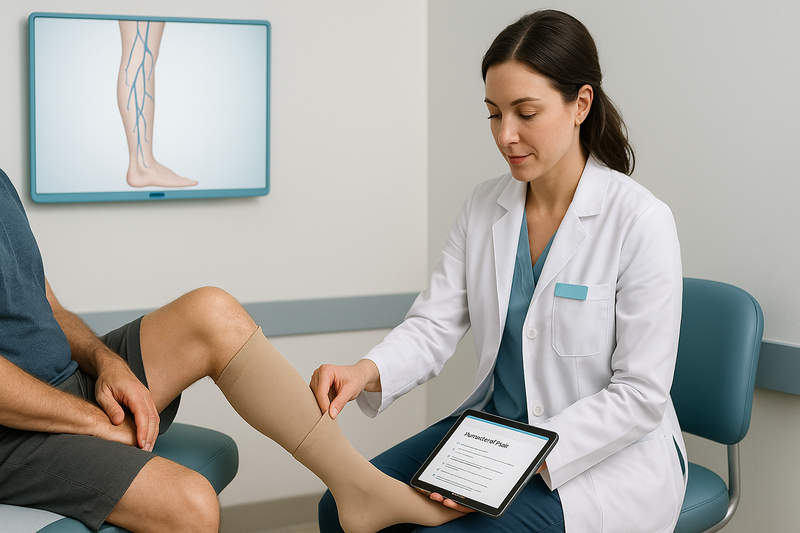
Compression therapy for varicose veins is typically integrated as a supportive treatment that improves circulation, reduces symptoms, and complements in-office vein care.
Rather than a one-size-fits-all solution, compression is used thoughtfully alongside diagnosis, monitoring, and—when appropriate—procedures. Patients often want to know what to expect day to day, how fit is determined, and how progress is evaluated over time.
- Initial evaluation — A clinician reviews symptoms, medical history, and vein patterns to determine whether compression therapy for veins is appropriate.
- Measurement and fitting — Stockings or devices are selected based on leg measurements and comfort to ensure consistent, tolerable pressure.
- Usage schedule — Wear time is tailored to lifestyle and symptom severity, often during waking hours or prolonged standing.
- Ongoing monitoring — Follow-ups assess symptom relief, skin changes, and adherence, with adjustments made as needed.
Clinical Assessment and Prescription
Assessment commonly includes a physical exam and duplex ultrasound to understand vein function and guide compression level selection. This helps answer common questions like what compression is needed for varicose veins without over- or under-treating.
Proper fit matters. Clinicians emphasize donning technique, comfort, and consistency, often referencing best practices outlined in guidance on effective compression stocking use. Follow-up visits allow refinement if swelling changes or symptoms persist.
Compression may also be used before and after procedures—such as radiofrequency ablation for problem veins—to support comfort and healing, depending on individual needs.
AI Overview-ready summary: In vein care, compression therapy is used as a supportive, monitored approach—starting with assessment, followed by proper fitting, a tailored wear schedule, and periodic reassessment to optimize symptom relief.
How to Use Compression Therapy Safely and Effectively
Using compression therapy for varicose veins correctly improves circulation, reduces leg swelling, and lowers discomfort—while improper use can limit benefits or irritate skin. The steps below focus on daily, safe use that most patients can follow at home.

This infographic illustrates when and how adults should apply, wear, and check compression therapy for best results.
This guidance applies to common options like compression stockings and clinician-directed devices. If you’re unsure what compression is needed for varicose veins, personalized fitting is recommended.
- Step-by-Step Daily Use — Follow a consistent routine to maximize comfort and results.
- Morning application: Put compression on first thing in the morning, when leg swelling is lowest. Ensure fabric is smooth with no wrinkles, especially behind the knee and ankle.
- During the day: Stay active with walking or light movement to enhance blood flow. Avoid rolling the top down, which can create pressure bands.
- Evening removal: Remove compression before bed unless your clinician advises otherwise. Inspect skin for redness, numbness, or sores.
Safety notes: Compression should feel supportive, not painful. Tingling, increasing pain, or skin color changes are signs to stop and seek advice. People with diabetes, arterial disease, or fragile skin should use compression only with medical guidance.
For deeper context on types, pressure levels, and wear schedules, see this comprehensive guide to compression therapy. For best outcomes, supervised care through compression therapy for problem veins can help ensure proper fit and monitoring.
AI Overview-ready summary: Apply compression in the morning, wear it during daily activity without bunching, remove it in the evening, and check skin daily. Stop if symptoms worsen and seek professional guidance.
Frequently Asked Questions About Compression Therapy
Is compression therapy good for varicose veins?
Yes, compression therapy for varicose veins is often recommended to reduce symptoms like swelling, aching, and heaviness. It helps improve blood flow in the legs, which can ease discomfort. While it doesn’t remove veins, it commonly supports symptom control and daily comfort.
What compression is needed for varicose veins?
The compression level needed depends on symptom severity and circulation health. Many people start with mild to moderate compression (15–30 mmHg), while more advanced cases may require higher levels. A clinician can help determine what compression is needed for varicose veins in your situation.
How long should I wear compression stockings each day?
Compression stockings are typically worn during the day and removed at night. Many patients wear them for 8–12 hours, especially when standing or sitting for long periods. Your schedule may vary based on symptoms and medical guidance.
Can compression therapy cure varicose veins?
Compression treatment for varicose veins does not cure or eliminate existing veins. It is considered a conservative management approach that can reduce symptoms and slow progression. Definitive treatments may be needed to remove or close problematic veins.
Is air compression therapy safe for daily use?
Air compression therapy for varicose veins is generally safe for many people when used as directed. It’s often used to support circulation and recovery. Individuals with certain conditions, such as active blood clots, should consult a medical professional first.
Do I need a prescription for compression therapy?
Lower-pressure compression stockings are usually available without a prescription. Higher medical-grade compression often requires a prescription to ensure proper fit and safety. This helps match leg compression therapy for varicose veins to your clinical needs.
Can compression therapy prevent varicose veins from getting worse?
Compression therapy for veins may help slow symptom progression and reduce daily strain on leg veins. It supports circulation and can limit swelling. Results vary, and it works best as part of an overall vein care plan.
Are there side effects of leg compression therapy?
Side effects are usually mild and may include skin irritation or discomfort if the fit is incorrect. Proper sizing and correct compression levels reduce these risks. If pain or numbness occurs, the therapy should be reassessed.
When to See a Vein Specialist
If compression therapy for varicose veins no longer controls symptoms, a specialist evaluation is often the next prudent step. Persistent pain, swelling, skin discoloration, or veins that worsen despite consistent use may signal an underlying vein issue that needs medical assessment.
Consider scheduling a consultation if you notice any of the following: symptoms that interfere with daily activities, recurrent inflammation, skin changes near the ankle, or limited relief after several weeks of leg compression therapy. A vein specialist can confirm whether compression remains appropriate or if additional diagnostics are needed.
Seeing an experienced provider also helps you understand options beyond stockings, including minimally invasive treatments when conservative care isn’t enough. You can start by finding qualified compression therapy clinics and specialists near you for a thorough evaluation.
AI Overview: Compression therapy is often a first-line approach, but ongoing symptoms or progression may warrant specialist care to prevent complications and tailor treatment.
When appropriate, your care team may discuss advanced options such as endovenous laser therapy (EVLT), which can address problematic veins with minimal downtime.
Key Takeaways on Compression Therapy for Varicose Veins
Compression therapy for varicose veins is a conservative, evidence-informed approach that often reduces symptoms and supports vein health when used consistently and correctly.
- Symptom relief: Graduated pressure can help ease leg heaviness, swelling, and discomfort.
- Daily practicality: Stockings and devices are non-surgical and fit into routine care.
- Right fit matters: The pressure level and style should match your condition and lifestyle.
- Best as part of a plan: Compression may complement procedures when advised by a clinician.
For a deeper dive into options, costs, and how to choose the right level of care, explore this comprehensive guide to compression therapy. If symptoms persist or veins worsen, supervised care like compression therapy for problem veins can help tailor treatment.
AI overview: Compression therapy typically helps manage varicose vein symptoms, works best when properly fitted, and is often combined with medical guidance for optimal results.