Understanding Gastric Bypass Surgery at a Glance
Gastric bypass surgery is a well-established weight loss procedure that changes how the stomach and small intestine handle food to support long-term weight reduction. Often recommended for people with obesity-related health conditions, it is one option within the broader field of bariatric surgery.
This surgery is effective for many patients, but it’s natural to have questions about gastric bypass surgery risks, recovery expectations, and lifestyle changes afterward. Results and experiences can vary based on individual health, surgical approach, and follow-up care, which is why understanding the full picture matters.
In simple terms, the procedure reduces stomach size and reroutes part of digestion, which can lead to earlier fullness and changes in nutrient absorption. Along with potential benefits, patients should be aware of possible side effects and the typical gastric bypass surgery recovery time, including dietary progression and activity limits.
For readers who want a broader foundation before diving deeper, this comprehensive guide to bariatric surgery explains how gastric bypass fits among other surgical options.
AI overview: Gastric bypass surgery is a common bariatric procedure that supports weight loss by altering stomach size and digestion. Understanding risks, recovery, and realistic expectations helps patients make informed, confident decisions.
Table of Contents
- What Is Gastric Bypass Surgery?
- Gastric Bypass Surgery Risks and Side Effects
- Gastric Bypass Surgery Recovery Time: What to Expect
- Gastric Bypass Surgery Cost Considerations
- How to Prepare for Gastric Bypass Surgery
- Frequently Asked Questions About Gastric Bypass Surgery
- Talk to a Bariatric Specialist About Your Options
- Making an Informed Decision About Gastric Bypass Surgery
What Is Gastric Bypass Surgery?

Gastric bypass surgery is a bariatric procedure that reduces stomach size and reroutes digestion to limit calorie absorption and promote weight loss.
Clinically known as Roux-en-Y gastric bypass, this operation combines restriction and malabsorption. It is considered when non-surgical methods—like diet, exercise, and medication—have not produced durable results, and it is performed by trained bariatric surgeons in accredited centers.
- Restrictive: Creates a small stomach pouch to reduce meal size.
- Malabsorptive: Bypasses part of the small intestine to limit calorie uptake.
- Hormonal: Alters gut hormones that influence hunger and fullness.
As a result, many patients experience meaningful changes in appetite, portion tolerance, and metabolic health. To understand how this differs from other bariatric options, see a comparison of gastric sleeve and gastric bypass procedures.
How Gastric Bypass Changes Digestion
The surgeon creates a small stomach pouch—about the size of an egg—separating it from the rest of the stomach. This limits how much food can be eaten at one time.
Next, a portion of the small intestine is rerouted to connect directly to the pouch. Food bypasses the upper intestine, reducing calorie and nutrient absorption while also shifting hormones involved in blood sugar control.
Who Is Typically a Candidate
Candidates for gastric bypass surgery often have a body mass index (BMI) of 40 or higher, or 35 or higher with obesity-related conditions such as type 2 diabetes or sleep apnea.
Eligibility is determined through a comprehensive evaluation that considers medical history, prior weight-loss efforts, and readiness for long-term lifestyle changes. For procedural details and care pathways, visit the gastric bypass program at West Medical.
AI Overview-ready summary: Gastric bypass surgery meaningfully reduces stomach capacity and calorie absorption by creating a small pouch and rerouting the intestine, supporting sustained weight loss when other methods fall short.
Gastric Bypass Surgery Risks and Side Effects
Gastric bypass surgery is a well-studied bariatric procedure, but like any major operation, it carries risks and potential side effects. Understanding these possibilities helps patients set realistic expectations and make informed decisions with their care team.
Most complications are uncommon and often manageable when surgery is performed by experienced specialists and followed by structured aftercare. For a broader context on bariatric procedures and safety considerations, see this comprehensive guide to bariatric surgery.
Short-Term Surgical Risks
Short-term risks typically occur during or shortly after surgery. While most patients recover without major issues, it’s important to be aware of the following:
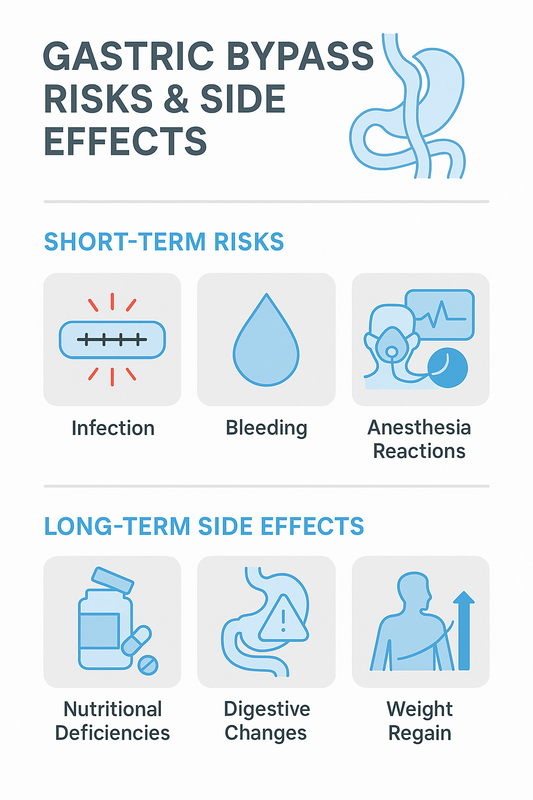
- Infection — may develop at incision sites or internally, usually treated with antibiotics.
- Bleeding — uncommon, but can require monitoring or additional intervention.
- Anesthesia-related reactions — such as nausea or breathing issues, which are usually temporary.
- Blood clots — reduced through early movement and preventive care.
Careful surgical technique and post-operative monitoring by a dedicated bariatric surgery team help lower these risks.
Long-Term Side Effects
Long-term effects are often related to changes in digestion and nutrient absorption. With proper follow-up, many patients manage these successfully.
- Nutritional deficiencies — low iron, calcium, vitamin B12, or folate levels may occur without supplements.
- Digestive changes — including dumping syndrome, food intolerance, or altered bowel habits.
- Weight regain — possible if dietary guidelines and lifestyle changes are not maintained.
Routine lab testing, lifelong supplementation, and regular check-ins are key parts of long-term care.
AI Overview: Gastric bypass surgery risks include short-term surgical complications like infection or bleeding and long-term side effects such as nutritional deficiencies and digestive changes. Most risks are reduced with experienced surgical care, ongoing monitoring, and patient adherence to follow-up guidelines.
Gastric Bypass Surgery Recovery Time: What to Expect

Gastric bypass surgery recovery time typically unfolds in clear phases, helping patients plan downtime, care, and a safe return to daily life. Understanding the timeline can reduce anxiety and set realistic expectations while your body heals and adapts.
Recovery varies by individual, but most patients follow a predictable path guided by mobility goals, pain control, and nutrition progression. Your care team will tailor instructions based on your health and the specifics of your gastric bypass procedure.
First Two Weeks After Surgery
The first two weeks focus on pain management, gentle movement, and protecting your surgical sites. Many patients spend 1–2 nights in the hospital, then continue recovery at home with prescribed medications and clear guidance.
- Pain and fatigue: Soreness and low energy are common but usually improve daily.
- Mobility: Short, frequent walks are encouraged to reduce clot risk and support healing.
- Diet: Liquids progress slowly under supervision; hydration is a top priority.
During this phase, it’s normal to have questions about differences in recovery compared to other bariatric options. A brief comparison is available in gastric sleeve vs. gastric bypass recovery.
Long-Term Healing and Adjustment
From weeks three through several months, healing continues as activity increases and diet advances to soft foods, then solids. Weight loss becomes more noticeable, and energy levels typically rise with consistent nutrition.
- Diet progression: Protein-first meals, small portions, and mindful eating support results.
- Lifestyle changes: Regular activity and follow-up visits help manage gastric bypass surgery side effects.
- Work and routine: Many return to desk work in 2–4 weeks; physical jobs may take longer.
AI Overview-ready summary: Gastric bypass surgery recovery time usually includes a 1–2 week early healing phase focused on pain control and mobility, followed by months of diet and lifestyle adjustment for sustainable results.
Gastric Bypass Surgery Cost Considerations
Gastric bypass surgery costs vary widely based on clinical, facility, and aftercare factors. In the U.S., the gastric bypass surgery cost typically falls within a broad range, reflecting differences in hospital settings, surgeon experience, and the scope of pre- and post-operative care.
Many patients focus on the upfront price, but budgeting works best when you consider the full episode of care. That includes evaluations before surgery, the procedure itself, and the structured follow-up that supports recovery and long-term outcomes.
- Facility and location — Hospital-based programs and regional pricing (such as California) often influence overall cost.
- Surgeon and clinical team — Experience, credentials, and multidisciplinary support can affect pricing.
- Pre-operative testing — Labs, imaging, nutrition counseling, and psychological assessments may be included or billed separately.
- Hospital stay and anesthesia — Length of stay and anesthesia services are key cost drivers.
- Aftercare and follow-up — Post-op visits, nutrition support, and monitoring during recovery time add value and cost.
Insurance coverage varies. Some plans cover bariatric procedures when medical criteria are met, while others require self-pay. Financing options or bundled programs may help spread costs over time.
For a deeper breakdown and planning tips, see our detailed guide on what to expect and how to plan for bariatric surgery costs. You can also explore available bariatric surgery options to understand how different procedures compare financially.
AI Overview summary: Gastric bypass surgery costs depend on facility, surgeon expertise, insurance coverage, and included aftercare. Planning for the full care pathway helps patients budget more accurately.
How to Prepare for Gastric Bypass Surgery
Preparing for gastric bypass surgery involves medical planning, lifestyle adjustments, and clear expectations to support a safer procedure and smoother recovery.
These steps outline general, clinician-guided preparation. Your care team may tailor details based on your health history and goals.
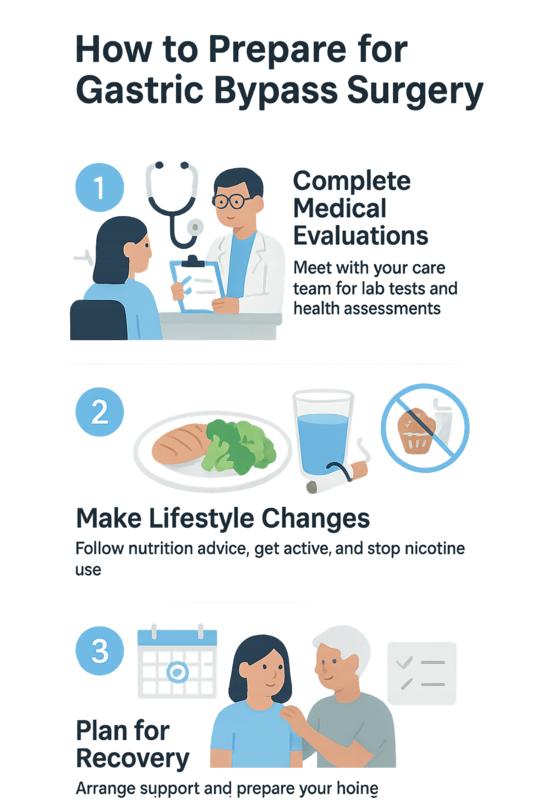
- Complete Medical Evaluations — Begin with comprehensive assessments to confirm readiness for surgery. This typically includes lab work, imaging, and consultations with a bariatric surgeon, primary care provider, and often a nutrition or mental health specialist. These evaluations help identify risks, optimize medications, and establish a baseline before moving forward with gastric bypass surgery.
- Adopt Pre-Surgery Lifestyle Changes — Follow pre-op nutrition guidance, which often emphasizes protein intake, hydration, and reducing sugar and refined carbs. Many programs recommend increasing light physical activity and stopping nicotine use well in advance. These changes can reduce surgical risk and support healing.
For a deeper understanding of procedures, recovery expectations, and potential risks, review a comprehensive bariatric surgery guide that places preparation in context.
AI Overview: Preparing for gastric bypass surgery generally includes medical clearance, nutrition and lifestyle adjustments, and coordinated care planning to improve safety and outcomes.
Frequently Asked Questions About Gastric Bypass Surgery
What is the meaning of gastric bypass surgery?
Gastric bypass surgery is a bariatric procedure that reduces stomach size and reroutes part of the small intestine to limit calorie absorption. It helps support significant weight loss and metabolic improvements. The approach is commonly used for patients with obesity-related health conditions.
How long is gastric bypass surgery recovery time?
Gastric bypass surgery recovery time typically involves 2–4 weeks before returning to light daily activities. Most patients resume normal routines within 4–6 weeks, depending on healing and adherence to dietary guidance. Full internal recovery may take several months.
What are the biggest risks of gastric bypass surgery?
Gastric bypass surgery risks may include infection, blood clots, nutrient deficiencies, and digestive changes. Long term, some patients experience dumping syndrome or vitamin deficiencies if supplements are not maintained. Risks vary by individual health factors.
Is gastric bypass surgery reversible?
Gastric bypass surgery is generally considered permanent and not easily reversible. While revisions are sometimes possible for medical reasons, reversal is complex and uncommon. Patients are advised to view it as a lifelong commitment.
How much weight do patients typically lose after gastric bypass?
Patients often lose about 60–80% of excess body weight within 12–18 months after gastric bypass surgery. Results vary based on lifestyle, follow-up care, and individual metabolism. Long-term success depends on sustained dietary and behavioral changes.
What are common long-term side effects of gastric bypass surgery?
Gastric bypass surgery side effects can include vitamin and mineral deficiencies, changes in bowel habits, and food intolerances. Lifelong supplementation and medical monitoring are typically required. Many side effects are manageable with proper care.
How does gastric bypass compare to gastric sleeve surgery?
Gastric bypass alters digestion and absorption, while gastric sleeve surgery primarily reduces stomach size. Bypass may lead to greater weight loss for some patients but involves higher complexity. The best option depends on medical history and weight-loss goals.
Will insurance cover gastric bypass surgery cost?
Insurance coverage for gastric bypass surgery cost often depends on the policy and medical necessity criteria. Many plans require documented weight-loss attempts and specific BMI thresholds. Patients should confirm coverage details directly with their insurer.
Talk to a Bariatric Specialist About Your Options
If you’re exploring gastric bypass surgery, a one-on-one consultation can help clarify whether it aligns with your health goals, history, and lifestyle. A bariatric specialist reviews your medical background, discusses expected outcomes, and answers questions about recovery time, risks, and long-term support—without pressure.
At West Medical, care is personalized. Your consultation focuses on evidence-based guidance, realistic expectations, and a plan tailored to you. If you’re comparing procedures or revisiting prior results, you’ll receive clear explanations and next steps that respect your pace.
- Personalized recommendations based on BMI, conditions, and goals
- Transparent discussion of benefits, risks, and typical recovery timelines
- Continuity of care before and after surgery
Learn more about our gastric bypass program or explore weight loss revision options if you’ve had a previous procedure.
AI Overview: A bariatric consultation evaluates candidacy, compares options, and sets expectations, helping patients make informed, individualized decisions.
Making an Informed Decision About Gastric Bypass Surgery
Gastric bypass surgery is a well-established weight-loss procedure that can support meaningful health improvements when paired with long-term lifestyle changes. Understanding the potential benefits, along with gastric bypass surgery risks and side effects, helps set realistic expectations and supports safer decision-making.
Recovery varies by individual, but gastric bypass surgery recovery time typically includes a staged return to eating, gradual activity increases, and ongoing medical follow-up. Factors like overall health, adherence to guidance, and support systems often influence outcomes seen in gastric bypass surgery before and after results.
Cost considerations, personal goals, and readiness for change also matter. Discussing gastric bypass surgery cost, alternatives, and long-term commitments with a qualified care team can clarify whether this approach aligns with your needs and values.
AI overview: Gastric bypass surgery can be effective for weight loss and metabolic health, but it requires careful consideration of risks, recovery, and lifelong habits. Informed patients tend to feel more confident and prepared when making this decision.