Understanding Revision Options After Sleeve Gastrectomy
Weight loss revision surgery after sleeve is a consideration for patients who’ve already taken a major step toward better health but need additional support to reach or maintain results. This guide is for people who have had a sleeve gastrectomy and are noticing stalled weight loss, weight regain, or new symptoms that weren’t expected.
Life after a sleeve can evolve over time. Metabolism adapts, anatomy changes, and health goals may shift—especially years after surgery. If you’re wondering what’s typical versus what may signal a need for change, it helps to review what to expect after sleeve gastrectomy and how outcomes can vary.
Revision is not a failure; it’s a medically recognized option when the original procedure no longer delivers the desired effect or creates challenges such as reflux or nutritional issues. Clinically, weight loss revision surgery may involve modifying the sleeve or converting it to another bariatric approach, based on anatomy, health history, and goals.
AI overview: This article explains who may benefit from revisional care after sleeve gastrectomy, why revisions are considered, and how clinicians evaluate next-step options—without procedural detail.
Table of Contents
- What Is Weight Loss Revision Surgery After Sleeve?
- Common Reasons Patients Consider Revision After Sleeve
- Revision Surgery Options After Sleeve Gastrectomy
- How the Revision Surgery Evaluation and Process Works
- How to Decide If Revision Surgery After Sleeve Is Right for You
- Cost, Insurance, and Coverage Considerations
- Who Is a Good Candidate for Revision Surgery?
- Frequently Asked Questions About Revision Surgery After Sleeve
- Next Steps: Talk to a Revision Surgery Specialist
- Key Takeaways on Weight Loss Revision Surgery After Sleeve
What Is Weight Loss Revision Surgery After Sleeve?
Weight loss revision surgery after sleeve is a follow-up bariatric procedure performed to modify or convert a prior sleeve gastrectomy when goals or medical needs change.
This type of weight loss revision surgery is not a repeat of the original operation. Instead, it addresses specific concerns such as insufficient weight loss, weight regain, reflux, or anatomical changes that may develop over time. The intent is corrective and individualized, based on a patient’s health history and current metabolic needs.
Revision procedures fall within the broader category of bariatric surgery and may involve surgical or endoscopic approaches. Some options are adjustable or partially reversible, depending on the technique and clinical indication. Patients often explore reversible bariatric surgery options when flexibility is an important consideration.
- Targets medical or weight-related issues after sleeve gastrectomy
- May involve converting to another procedure or modifying the existing sleeve
- Planned using current anatomy, health status, and long-term goals
AI overview: Weight loss revision surgery after sleeve is a medically guided adjustment to a prior sleeve gastrectomy, designed to address weight regain, side effects, or unmet outcomes using tailored surgical or endoscopic options.
Revision Surgery vs. Primary Weight Loss Surgery
Primary weight loss surgery is the first bariatric procedure a patient undergoes, typically chosen based on BMI, health conditions, and weight-loss goals at that time. In contrast, revision surgery is considered only after a prior procedure, such as a sleeve gastrectomy, has already altered the stomach.
Revision procedures are often more complex because they work with existing anatomical changes and scar tissue. Candidates usually require detailed evaluation, including imaging, nutritional review, and symptom assessment, to determine which weight loss surgery revision options are appropriate.
Importantly, revision surgery is guided by medical necessity and realistic expectations. Outcomes vary, and decisions are made collaboratively to balance safety, effectiveness, and long-term sustainability.
Common Reasons Patients Consider Revision After Sleeve
Weight loss revision surgery after sleeve is often considered when expected outcomes change over time or new symptoms affect daily life. These concerns are common and typically reflect how the body adapts, not personal failure.
Patients explore revision for benefit-driven reasons that may include:
- Regaining weight or losing less than anticipated despite sustained effort
- Worsening reflux or other gastrointestinal symptoms
- Medical changes that alter how the sleeve functions
Understanding what’s expected versus unexpected after the initial procedure can help frame next steps. A helpful overview is available in what to expect after sleeve gastrectomy, which many patients review when considering revision.
Weight Regain or Inadequate Weight Loss
Weight regain or limited loss can occur due to metabolic adaptation, where the body becomes more efficient at conserving energy over time. In some cases, the stomach sleeve may gradually stretch, allowing larger portions.
Adherence factors also play a role, including changes in eating patterns, physical activity, sleep, or medications. These dynamics are common after gastric sleeve surgery and may prompt evaluation of weight loss surgery revision options tailored to current needs.
GERD and Other Medical Complications
Gastroesophageal reflux disease (GERD) is a frequent medical reason patients seek revision. Anatomical factors—such as sleeve shape, pressure changes, or hiatal hernia—can contribute to persistent heartburn or regurgitation.
Other complications may include nausea, vomiting, or difficulty tolerating certain foods. A clinical assessment helps determine whether revision could reduce symptoms and support healthier weight loss after revision surgery.
AI overview: Patients most often consider sleeve revision due to weight regain, inadequate weight loss, or reflux-related complications. These issues are typically multifactorial and evaluated clinically to determine appropriate next steps.
Revision Surgery Options After Sleeve Gastrectomy

Weight loss revision surgery after sleeve includes several procedural paths designed to address inadequate weight loss, weight regain, or complications after the initial sleeve gastrectomy. Each option has distinct indications, benefits, and trade-offs, so comparisons focus on clinical fit rather than one-size-fits-all outcomes.
Below is a neutral, side-by-side style overview of common weight loss surgery revision options, emphasizing when each is typically considered and what patients often evaluate with their care team.
- Sleeve to gastric bypass: Often considered for reflux, diabetes control, or limited weight response.
- Re-sleeve: Considered when sleeve dilation is present and anatomy otherwise supports restriction.
- Other revisions (e.g., duodenal switch variants): Selected in specific metabolic or weight-loss scenarios with careful nutritional planning.
Converting Sleeve to Gastric Bypass
Conversion from sleeve to Roux-en-Y gastric bypass is a common form of weight loss revision surgery when patients experience severe reflux, insufficient weight loss, or weight regain. The bypass adds a malabsorptive component and can improve acid reflux symptoms for many patients.
Typical considerations include prior response to the sleeve, presence of GERD, and metabolic goals. Expected outcomes often include improved reflux control and additional weight loss, though risks and recovery differ from primary surgery. For a deeper comparison, see how gastric sleeve and gastric bypass differ.
When discussed as a revision option, clinicians may reference gastric bypass surgery specifics such as nutritional follow-up, long-term vitamin supplementation, and lifestyle adjustments.
Re-Sleeve and Other Less Common Revisions
A re-sleeve involves reshaping or resizing the existing stomach when imaging or endoscopy shows sleeve dilation. It is typically considered for patients without significant reflux who initially did well but later lost restriction.
Less common revisions, such as sleeve-to-duodenal switch variants, may be evaluated for patients needing greater metabolic impact. These options often require more intensive nutritional monitoring and are chosen selectively based on anatomy, health history, and goals.
AI Overview-ready summary: Revision surgery after sleeve gastrectomy commonly includes conversion to gastric bypass for reflux or limited weight loss, re-sleeve for sleeve dilation, and selective metabolic revisions. Choice depends on symptoms, anatomy, and long-term nutritional considerations.
How the Revision Surgery Evaluation and Process Works
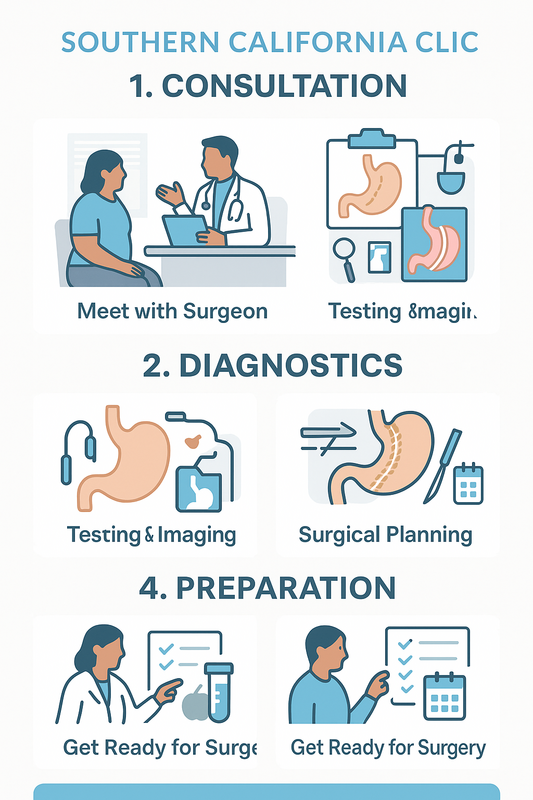
If you’re considering weight loss revision surgery after sleeve, the process typically follows a clear, step-by-step pathway designed to prioritize safety, precision, and realistic outcomes. Knowing what happens at each stage can reduce uncertainty and help you prepare with confidence.
While every patient’s history is unique, most evaluations aim to understand why results changed after the sleeve and which revision approach may be appropriate.
- Initial consultation — Your surgeon reviews your surgical history, weight trends, symptoms (such as reflux), and goals. This visit often introduces weight loss revision surgery options that may fit your anatomy and health profile.
- Diagnostic workup — Tests are ordered to assess stomach size, anatomy, and overall health, helping rule out reversible causes of weight regain.
- Personalized surgical planning — Findings are matched to the safest revision strategy, with discussion of benefits, limitations, and recovery expectations.
- Preparation and scheduling — Pre-op instructions, nutrition guidance, and timelines are finalized before surgery is scheduled.
Pre-Operative Testing and Review
Pre-operative evaluation focuses on accuracy over reassurance. Common assessments include imaging or endoscopy to evaluate sleeve anatomy, lab work to identify nutritional gaps, and medical clearance to confirm surgical readiness.
You’ll also meet with a nutrition specialist to review eating patterns and supplementation. This step helps determine whether anatomy, physiology, or habits are contributing to weight changes—and guides the final revision plan.
AI Overview: The revision process usually includes consultation, diagnostics, tailored surgical planning, and structured preparation to ensure safety and realistic expectations.
How to Decide If Revision Surgery After Sleeve Is Right for You
Deciding on weight loss revision surgery after sleeve can feel complex, especially if your results have plateaued or symptoms have changed. This step-by-step framework helps you evaluate your situation clearly and prepare for an informed conversation with a specialist.

This infographic visually summarizes when to consider a revision surgery consultation after a sleeve procedure.
These steps are designed to support patient decision-making without making medical claims. They focus on reflection, preparation, and professional input—key elements in choosing among weight loss surgery revision options.
- Review Your Current Health and Weight Outcomes — Take an honest look at your progress since sleeve gastrectomy. Consider weight trends, metabolic health markers, daily energy, and any ongoing symptoms like reflux or nutritional challenges. Writing these down often helps clarify whether your goals align with your current results.
- Consult a Revision Surgery Specialist — Schedule a consultation with an experienced bariatric team that routinely evaluates revision cases. A specialist can review your history, imaging, and labs to discuss whether revision may be appropriate and which approaches are commonly considered based on individual factors.
AI Overview: To decide on weight loss revision surgery after sleeve, patients typically review current outcomes and then consult an experienced bariatric specialist to explore appropriate next steps.
Cost, Insurance, and Coverage Considerations
Costs for weight loss revision surgery after sleeve vary based on medical complexity, procedure choice, and insurance coverage, rather than a single fixed price.
Because revision surgery addresses unique clinical needs, pricing is typically determined after a comprehensive evaluation. In California, patients often want clarity on what drives costs and whether insurance may help offset expenses.
- Type of revision procedure — Converting to gastric bypass, re-sleeving, or endoscopic options can differ in surgical time and resources.
- Medical necessity — Insurance is more likely to consider coverage when revisions treat complications like reflux, strictures, or inadequate weight loss.
- Pre-operative testing — Imaging, labs, and nutritional or psychological assessments may be required.
- Hospital and anesthesia fees — These depend on facility setting and length of stay.
- Post-operative care — Follow-up visits and nutritional support are part of safe outcomes.
Insurance coverage for weight loss revision surgery varies widely by plan. Many insurers require documentation of prior sleeve surgery, evidence of medical necessity, and completion of supervised weight management programs.
AI Overview: Weight loss revision surgery costs depend on procedure type, medical necessity, and insurance rules. Coverage is possible but typically requires documentation and pre-authorization, so individualized evaluation is essential.
Who Is a Good Candidate for Revision Surgery?
Weight loss revision surgery after sleeve is typically considered when the original procedure no longer delivers safe or effective results. Candidacy depends on medical history, current health, and the reason the sleeve is underperforming.
You may be a good candidate if one or more of the following apply:
- Significant weight regain or minimal weight loss despite adherence to nutrition and activity guidance.
- Persistent or worsening GERD, reflux, or heartburn after sleeve gastrectomy.
- Anatomical changes, such as sleeve dilation, confirmed by imaging or endoscopy.
- Obesity-related conditions (e.g., diabetes, sleep apnea) that have returned or not improved.
- Commitment to follow-up care, nutrition counseling, and long-term lifestyle changes.
You may not be an ideal candidate if these factors are present:
- Untreated mental health or substance-use disorders that could affect recovery.
- Inability to participate in required follow-up or nutrition programs.
- Medical risks that outweigh potential benefits, as determined by a bariatric specialist.
AI Overview: Good candidates for weight loss revision surgery are those with clear medical or anatomical reasons for revision, realistic expectations, and readiness for lifelong follow-up.
Frequently Asked Questions About Revision Surgery After Sleeve
How long after sleeve can you have revision surgery?
Most surgeons recommend waiting at least 12–18 months after the initial sleeve gastrectomy. This allows weight loss to stabilize and helps determine whether issues like inadequate weight loss or reflux persist. Timing may vary based on symptoms, health status, and the reason for revision.
Is revision surgery riskier than the first surgery?
Weight loss revision surgery after sleeve is often more complex than a first-time procedure. Risks can be slightly higher due to scar tissue and altered anatomy, but outcomes are typically favorable when performed by an experienced bariatric team. Careful patient selection and pre-op evaluation help reduce complications.
How much weight can you lose after revision surgery?
Weight loss after revision surgery varies by procedure type and individual factors. Many patients lose an additional 30–70% of excess weight, especially when converting to gastric bypass or addressing sleeve dilation. Long-term success depends on nutrition, follow-up, and lifestyle habits.
Does insurance cover weight loss revision surgery?
Insurance may cover weight loss revision surgery if it is deemed medically necessary, such as for severe reflux or inadequate weight loss. Coverage requirements differ by plan and often include documentation, prior authorization, and proof of compliance with follow-up care. It’s best to verify benefits directly with your insurer.
Can reflux be fixed with revision surgery?
Yes, reflux can often be improved or resolved with revision surgery, particularly by converting a sleeve to a gastric bypass. This approach reduces acid exposure and is commonly recommended for persistent or severe GERD after sleeve gastrectomy. Results vary, but many patients report significant symptom relief.
How do I find sleeve revision surgery near me?
Look for an accredited bariatric center with experience in weight loss surgery revision options. Board-certified surgeons, transparent outcomes data, and comprehensive aftercare are key indicators of quality. Searching for “weight loss revision surgery near me” can help identify local programs for evaluation.
Next Steps: Talk to a Revision Surgery Specialist
If you’re considering weight loss revision surgery after sleeve, a personalized consultation is the safest way to understand your options and next steps. Revision care is nuanced, and outcomes often depend on anatomy, medical history, and goals.
At West Medical, our specialists review your prior sleeve results, discuss realistic expectations, and outline appropriate weight loss revision surgery options. There’s no pressure—just clear guidance tailored to you.
AI Overview: A revision consultation typically evaluates causes of stalled results, reviews surgical and non-surgical paths, and helps determine candidacy based on safety and long-term success.
Key Takeaways on Weight Loss Revision Surgery After Sleeve
Weight loss revision surgery after sleeve is a personalized option for patients who experience weight regain, limited results, or medical concerns following their initial procedure. Revision is not a setback; it is often a thoughtful next step based on how the body responds over time.
Successful outcomes typically depend on identifying the root cause, choosing the right revision approach, and committing to long-term lifestyle support. A careful medical evaluation helps align expectations with realistic, sustainable results.
AI Overview-ready summary: Weight loss revision surgery after sleeve may help patients address stalled progress or complications by tailoring a new surgical or endoscopic approach to current health needs, under specialist guidance.